Rapamycin for Cardiovascular Health: Prevention and Treatment Potential

Cardiovascular disease remains the leading cause of mortality worldwide, with aging serving as the primary risk factor. As we age, the heart and blood vessels undergo progressive changes—including increased arterial stiffness, impaired relaxation (diastolic dysfunction), and a decline in endothelial health—often long before clinical symptoms appear. Rapamycin, an FDA-approved compound originally used in organ transplantation, has emerged as the most robust and reproducible “geroprotector” in preclinical studies for reversing these age-related declines.
By modulating the mTOR (mechanistic target of rapamycin) pathway, particularly the mTORC1 complex, rapamycin shifts cellular activity from growth and inflammation toward maintenance, repair, and autophagy. This article explores the dual potential of rapamycin in both preventing cardiovascular aging and treating established heart conditions.
The Role of mTOR in Heart Aging
The mTOR pathway acts as a central nutrient sensor that integrates signals from growth factors and energy levels to regulate cell growth and metabolism. In the aging heart, mTORC1 activity often becomes inappropriately hyperactivated, contributing to tissue stiffness, impaired cellular repair, and chronic low-grade inflammation.
Research across diverse species, including yeast and fruit flies, shows that inhibiting mTORC1 with rapamycin mimics caloric restriction. Studies in mice and dogs confirm these findings. This process extends both lifespan and “healthspan”. In the cardiovascular system, this inhibition reduces the energetic burden on cells and facilitates the clearance of damaged organelles.
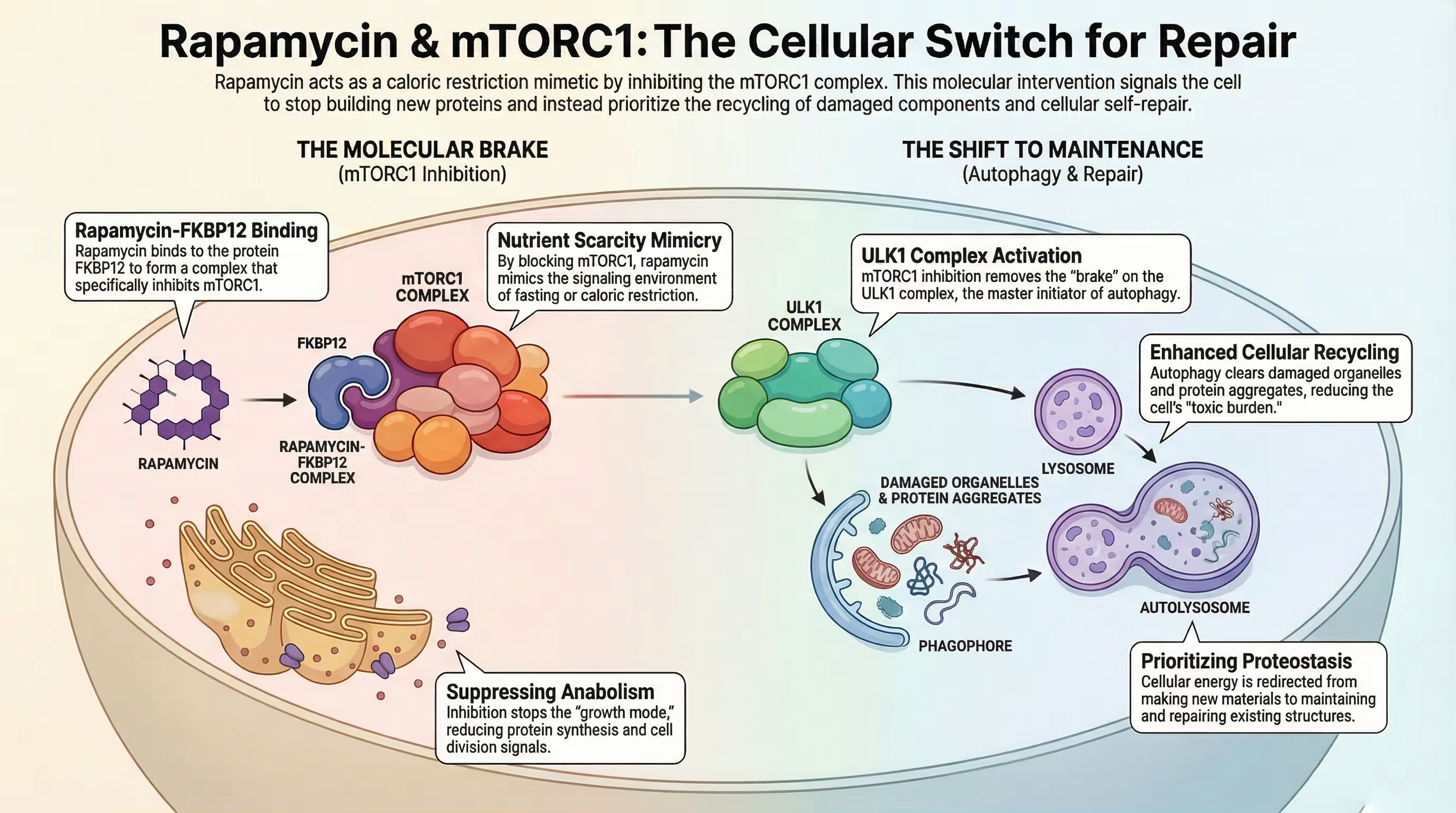
How mTORC1 Inhibition Protects the Myocardium
mTORC1 inhibition protects the myocardium by shifting cellular activity from growth and inflammation toward maintenance, repair, and internal cleaning processes. This protection is primarily achieved through the following mechanisms:
1. Activation of Autophagy and Mitophagy
The most critical protective effect of mTORC1 inhibition is the stimulation of autophagy (cellular self-eating) and mitophagy (the specific clearance of damaged mitochondria).
- Removal of Cellular “Trash”: Under normal conditions, mTORC1 suppresses autophagy by phosphorylating the ULK1 complex. Inhibiting mTORC1 removes this “brake,” allowing cardiomyocytes to degrade and recycle misfolded proteins and dysfunctional organelles that are otherwise toxic to the heart.
- Mitochondrial Quality Control: Mitophagy removes damaged mitochondria that have low membrane potential. This prevents the leak of reactive oxygen species (ROS), which can cause oxidative damage and trigger cell death pathways like apoptosis or necroptosis.
2. Regression of Pathological Hypertrophy
Hyperactivation of the mTORC1 pathway is a major driver of pathological cardiac hypertrophy (thickening of the heart walls) in response to stress like hypertension or pressure overload.
- Reducing Energetic Burden: By inhibiting the downstream effectors (S6K1 and 4E-BP1), mTORC1 inhibition reduces the massive energetic demand of excessive protein synthesis.
- Restoring Functional Balance: Studies using animal models of pressure overload show promising results for rapamycin. This treatment can effectively regress established cardiac hypertrophy. It also improves overall heart function. These benefits occur even when treatment begins after heart failure has already developed.
3. Improvement of Diastolic and Endothelial Function
Aging leads to diastolic dysfunction, where the heart becomes too stiff to relax and fill properly.
- Reducing Passive Stiffness: mTORC1 inhibition with rapamycin has been shown to persistently reverse age-related increases in myocardial stiffness. It achieves this by selectively modifying the composition of the arterial wall, specifically by decreasing collagen accumulation and cross-linking caused by advanced glycation end-products (AGEs).
- Endothelial Health: It improves nitric oxide (NO) bioavailability, which helps blood vessels dilate more effectively, reducing the workload on the heart and improving oxygen delivery to the myocardium.
4. Protection Against Ischemic Injury
During a heart attack (ischemia) or the restoration of blood flow (reperfusion), mTORC1 inhibition serves as a cardioprotective shield.
- Limiting Infarct Size: By maintaining a healthy population of mitochondria through autophagy, the heart is better equipped to survive periods of low oxygen.
- Anti-Apoptotic Effects: Activated autophagic flux inhibits apoptosis (programmed cell death) in cardiomyocytes, preserving the muscle mass necessary for the heart to continue pumping.
5. The “Rapamycin Memory” Effect
A unique feature of this protection is its persistence. Preclinical research demonstrates that a short course of mTORC1 inhibition can lead to long-lasting improvements in cardiac function that remain for months after the drug is discontinued. This suggests that “re-tuning” the mTOR pathway may biologically rejuvenate the heart rather than just providing a temporary fix.
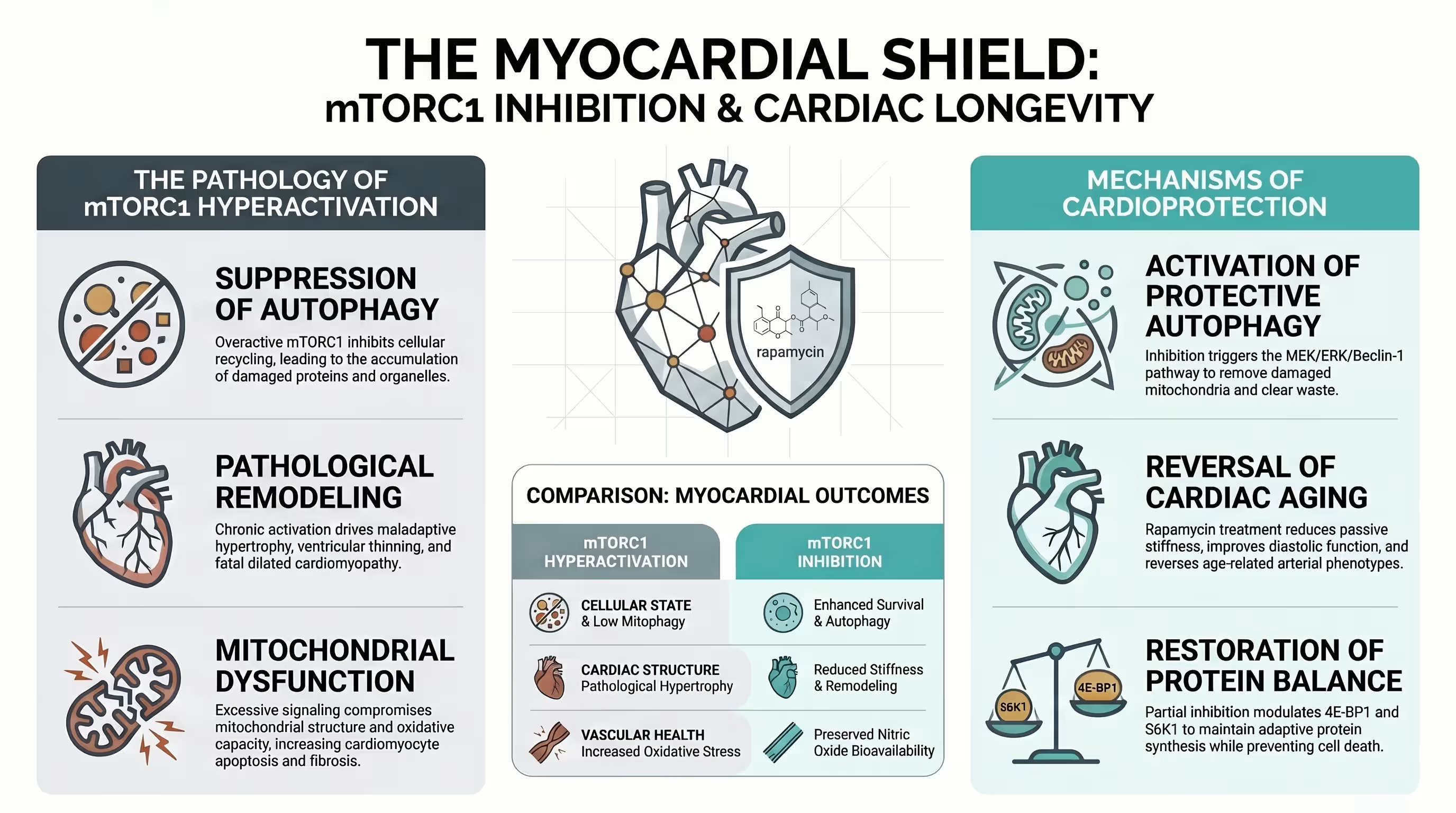
Reversing Vascular and Structural Decline
One of the most exciting prospects for rapamycin is its ability to reverse the biological clock of the heart and arteries.
- Vascular Rejuvenation: In aged mice, short-term rapamycin treatment reverses age-related vascular dysfunction and oxidative stress. It improves nitric oxide (NO) bioavailability, which is essential for keeping blood vessels flexible and responsive.
- Persistent Structural Benefits: Research shows that an 8-week rapamycin course in aged mice improves diastolic function and myocardial stiffness. These benefits persist for two months after the drug is stopped. This “rapamycin memory” suggests that intermittent dosing may provide long-term protection.
- Reduced Arterial Stiffness: Rapamycin has been shown to reduce stiffness in large elastic arteries. It selectively modifies the composition of the arterial wall. This process works by decreasing the accumulation of collagen. Additionally, it reduces the presence of advanced glycation end-products (AGEs).
Treating Atherosclerosis and Heart Failure
Beyond prevention, rapamycin possesses multifaceted mechanisms for addressing advanced cardiovascular pathologies.
Combating Atherosclerosis
Atherosclerosis is a chronic inflammatory disease characterized by the buildup of plaques in the arterial wall. Rapamycin targets several stages of this process:
- Plaque Stability: It enhances the stability of atherosclerotic plaques by decreasing the necrotic core and attenuating local inflammation.
- Foam Cell Inhibition: Rapamycin reduces the formation of “foam cells” by decreasing cholesterol uptake and synthesis while enhancing cholesterol efflux from plaque-resident macrophages.
- Inhibiting Restenosis: Due to its anti-proliferative effects, rapamycin is already successfully used in drug-eluting stents to prevent the re-narrowing of arteries after surgical procedures.
Addressing Heart Failure and Hypertrophy
Heart failure with preserved ejection fraction (HFpEF) is a growing concern for the elderly, driven largely by ventricular stiffening.
- Regression of Hypertrophy: In animal models of pressure overload, rapamycin regresses established cardiac hypertrophy and improves overall heart function.
- Autophagy as a Protective Shield: By stimulating autophagy, rapamycin helps cardiomyocytes degrade misfolded proteins. It also clears out dysfunctional mitochondria. This process protects the heart from injury during stress or ischemia.

| Feature | Rapamycin (Geroprotector) | Traditional Treatments |
|---|---|---|
| Primary Goal | Rejuvenate biological function | Manage specific symptoms |
| Target | mTOR signaling & Autophagy | Blood pressure, cholesterol |
| Effect on Aging | Delays/reverses fundamental aging | No direct impact on aging rate |
| Persistent Benefit | Shows “rapamycin memory” after cessation | Typically requires life-long daily use |
| Stent Application | Used in drug-eluting stents | Standard metal stents |
TABLE: Rapamycin vs. Traditional Heart Interventions
Human Evidence: Moving from Mice to Men
While preclinical data is extensive, human clinical trials are now providing the first “proof-of-concept” for rapamycin’s cardiovascular benefits.
A recent pilot study found that taking just 1 mg of rapamycin daily for 8 weeks led to measurable improvements in diastolic filling and endothelial function. The study participants’ hearts behaved structurally and functionally more like those of individuals 10 to 15 years younger.
Furthermore, the PEARL trial is the longest randomized controlled trial of rapamycin in humans to date. It demonstrated that low-dose, intermittent rapamycin is safe for healthy aging cohorts. The trial also noted an interesting “female-benefit bias” in the results. Women showed significant improvements in both lean muscle mass and overall quality of life.
Therapeutic Applications: Rapamycin in Modern Cardiology
Sirolimus-Eluting Stents: Preventing Restenosis
The introduction of sirolimus-eluting stents (SES) has revolutionized the field of interventional cardiology by significantly reducing the incidence of in-stent restenosis compared to bare-metal stents. These devices were the first drug-eluting stents approved by the FDA, specifically designed to address the problem of lumen re-narrowing after angioplasty.
Clinical trials like the RAVEL and SIRIUS studies show impressive results for SES. These stents remarkably eliminate the occurrence of restenosis. They also reduce the need for repeated revascularization procedures. Some concerns regarding late stent thrombosis still exist. However, research indicates that biocompatible polymers allow for the controlled release of sirolimus. This localized delivery maintains vessel patency for several years.
Managing Cardiac Hypertrophy and Pressure Overload
Rapamycin has shown profound potential in regressing established cardiac hypertrophy caused by chronic mechanical stress or pressure overload. Preclinical studies show that rapamycin attenuates the thickening of heart walls by inhibiting the hyperactivated mTORC1 pathway. This attenuation is largely driven by the stimulation of autophagy, which clears damaged proteins and organelles that accumulate in the stressed myocardium.
The benefits of this treatment appear to have a “rapamycin memory” effect; in aged mice. The reduction in hypertrophy and the improvement in diastolic function persist for months even after the medication is discontinued. The partial pharmacological inhibition provides a “geroprotective” shield that prevents the transition from compensatory hypertrophy to overt heart failure.
Rapamycin vs. Statins: Complementary or Alternative?
Rapamycin and statins are no longer viewed as mere alternatives. Instead, they are increasingly considered complementary therapies in cardiovascular care. Statins remain the “gold standard” for preventing late-stage events like thrombosis. However, rapamycin offers unique benefits. It can reverse biological aging markers and correct aberrant cellular activities. These are specific targets that statins do not address. Consequently, a combination approach is viewed as a reasonable strategy. This involves pairing an mTOR inhibitor with a statin or a PCSK9 inhibitor. This method aims to maximize anti-atherosclerotic benefits while minimizing metabolic risks.

Implementation: Low-Dose Rapamycin for Heart Longevity
The translation of rapamycin for cardiovascular longevity requires a major shift in strategy. It must move from chronic high-dose protocols toward low-dose, intermittent regimens. Preclinical research spans diverse species, from yeast to non-human primates. These studies demonstrate that high daily doses can be toxic. However, partial inhibition of mTORC1 through lower doses effectively triggers biological repair mechanisms. This shift in implementation aims to capture the heart-rejuvenating benefits of the drug. Crucially, it bypasses the severe metabolic and immunological trade-offs seen in clinical transplant settings.
Emerging research indicates that low-dose, intermittent regimens (e.g., 3–10 mg once weekly) may minimize these risks while maintaining geroprotective benefits. For example, while rapamycin can cause a reversible rise in blood lipids, it simultaneously induces protective mechanisms like cholesterol efflux, which can counteract the risks of atherosclerosis.
Conclusion
Rapamycin stands as a promising therapeutic agent with the potential to transform cardiovascular medicine from a focus on treating late-stage events to a focus on biological rejuvenation. By targeting the fundamental drivers of aging, it offers a path toward preventing arterial stiffness and diastolic decline while stabilizing advanced disease like atherosclerosis. As ongoing trials like TRIAD (dogs) and RESTOR (humans) continue to refine dosing protocols, we move closer to establishing rapamycin as a cornerstone of healthy longevity.

Rapamycin works by inhibiting the mTORC1 pathway, which shifts the heart’s cellular activity from growth and inflammation toward repair and maintenance. It triggers “autophagy”—a process where cells clear out damaged proteins and dysfunctional mitochondria—effectively “cleaning” the heart tissue at a cellular level.
Yes, preclinical research suggests that rapamycin can reduce arterial stiffness by modifying the composition of the arterial wall. It helps decrease collagen accumulation and cross-linking caused by advanced glycation end-products (AGEs), leading to more flexible and responsive blood vessels.
This refers to the phenomenon where the cardiovascular benefits of rapamycin persist even after the medication is stopped. Studies in animal models showed that a short course of treatment provided long-lasting improvements in heart function and diastolic filling for months after the final dose.
These treatments are generally viewed as complementary rather than alternatives.
Statins remain the “gold standard” for managing cholesterol and preventing blood clots. However, rapamycin targets the underlying biological aging of the heart and blood vessels. This addresses specific areas that traditional statins do not cover.
Rapamycin shows significant potential in treating heart failure with preserved ejection fraction. It works by regressing pathological cardiac hypertrophy. This process helps thin the thickened heart walls. By stimulating autophagy, the drug helps heart muscles survive stress. It also allows the heart to handle high blood pressure more effectively.
For longevity and heart health, researchers are shifting away from high daily doses used in transplant medicine toward “low-dose, intermittent” regimens. Common experimental protocols often involve a once-weekly dose (typically 3–10 mg). This maximizes heart-rejuvenating benefits while minimizing potential side effects.
Yes. Research indicates that rapamycin enhances the stability of atherosclerotic plaques by decreasing their necrotic core and reducing local inflammation. It also inhibits the formation of “foam cells,” which are key contributors to the buildup of plaque in the arteries.
Rapashop sources Rapamycin tablets, manufactured by global pharmaceutical companies with Internationally recognized “Good Manufacturing Standards”.
Resource links
Targeting the biology of aging with mTOR inhibitors
The mTOR Signaling Pathway: Key Regulator and Therapeutic Target for Heart Disease
Influence of rapamycin on safety and healthspan metrics after one year: PEARL trial results
New Insights Into the Role of mTOR Signaling in the Cardiovascular System
mTOR Inhibition and Cardiovascular Diseases: Dyslipidemia and Atherosclerosis
Autophagy in Heart Failure: Insights into Mechanisms and Therapeutic Implications
Safety and efficacy of rapamycin on healthspan metrics after one year: PEARL Trial Results
Targeting the biology of aging with mTOR inhibitors
Rapamycin for longevity: the pros, the cons, and future perspectives
Sirolimus-eluting coronary stents: a review
MTORC1 regulates cardiac function and myocyte survival through 4E-BP1 inhibition in mice