Topical Rapamycin for Skin Aging: Topical Applications and Results

The pursuit of skin longevity has moved aggressively past surface-level hydration and chemical resurfacing. Clinicians and biohackers are now targeting the specific molecular pathways that govern how dermal cells age, mutate, and eventually shut down. Skin aging is driven by a deep cellular failure: the accumulation of senescent “zombie” fibroblasts, the exhaustion of stem cell populations, and the degradation of the extracellular matrix (ECM).
At the center of this cellular decline is the mTOR (mechanistic target of rapamycin) pathway. When chronically overactivated by nutrient abundance, UV radiation, and intrinsic aging, mTOR drives skin cells into permanent senescence. Today, prescription rapamycin (sirolimus) is being heavily scrutinized for its ability to block this pathway. We are going to bypass the basic definitions and dive straight into the clinical data, off-label user protocols, and biological mechanisms driving the use of topical rapamycin for skin longevity.
How does Rapamycin inhibit the mTORC1 pathway to reverse skin aging?
Rapamycin targets skin aging by directly binding to the FKBP12 protein to inhibit the mTORC1 signaling pathway. This inhibition halts cellular over-proliferation, forces the cell into a repair state, and triggers autophagy to clear out damaged proteins and the toxic senescent cells that degrade dermal collagen.
Senescent dermal fibroblasts are the primary culprits behind aging skin. As these cells accumulate DNA damage from factors like UV radiation, they stop dividing but refuse to die. Instead, they secrete a toxic, inflammatory cocktail known as the Senescence-Associated Secretory Phenotype (SASP). Recent epilipidomic profiling reveals that senescent fibroblasts secrete specific oxidized lipids, such as lysophosphatidylcholines, which suppress local immune clearance and fuel chronic low-grade inflammation in the skin.
Topical rapamycin intervenes by essentially putting the brakes on the cellular machinery that produces this toxic SASP. By inhibiting mTOR, rapamycin reactivates autophagy—the cellular waste disposal system. This clears out the lysophosphatidylcholines and oxidized proteins, allowing the dermal fibroblasts to regain their youthful “priming” and re-establish healthy communication with surrounding skin cells.
What are the proven rapamycin results for wrinkles and photoaging?
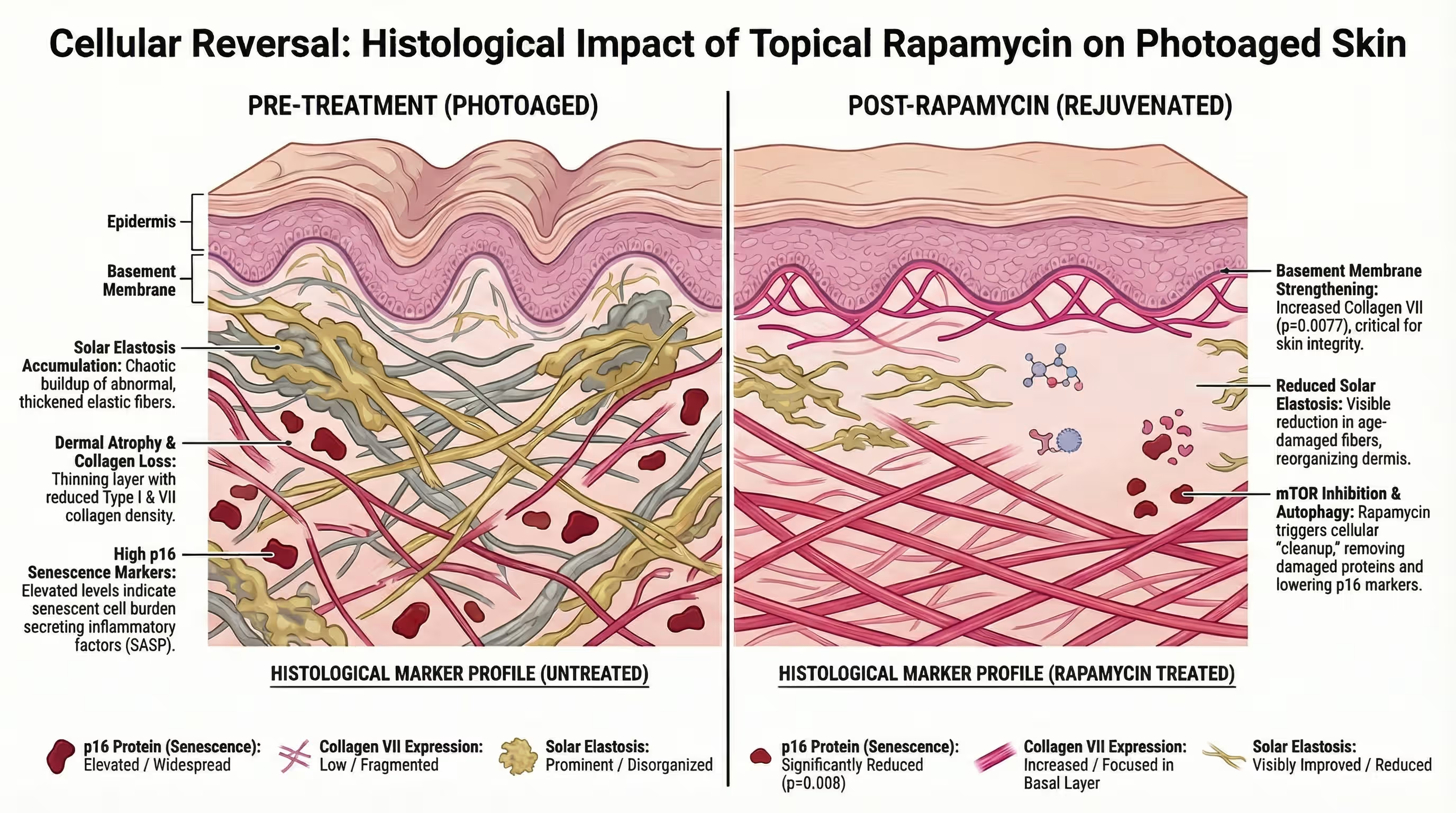
Clinical rapamycin results show a significant drop in the aging biomarker p16INK4A and a measurable increase in collagen VII protein within eight months of topical use. Visually, patients display decreased wrinkle depth, reduced dermal sagging, and a visibly more even skin tone.
The most robust human data comes from a landmark placebo-controlled clinical trial conducted at Drexel University and published in GeroScience. Researchers instructed participants over the age of 40 to apply a 10 μM sirolimus rapamycin cream every one to two days to one hand, while applying a placebo to the other.
After eight months, the biopsies revealed a profound biological shift. The rapamycin-treated hands showed a statistically significant reduction in p16INK4A, a primary molecular marker of cellular senescence. Skin with lower p16 levels exhibits fewer wrinkles and resists the dermal atrophy that causes elderly skin to tear easily. Furthermore, rapamycin increased the production of collagen VII, the critical protein responsible for anchoring the epidermis to the deeper dermis, thereby restoring structural integrity.
Beyond intrinsic aging, rapamycin heavily protects against UVA-induced photoaging. Fibroblasts exposed to UVA typically suffer impaired lysosomal function, elevated p53 stress proteins, and an accumulation of phosphorylated HSP27. Rapamycin protects these skin fibroblasts from UVA damage by activating autophagic clearance and downregulating both p53 and phosphorylated HSP27, effectively rescuing the skin from genotoxic stress.
Topical rapamycin before and after: What do real users report?
Topical rapamycin before and after results typically emerge slowly, taking 4 to 8 months to manifest structural changes. Real-world users tracking their progress note subtle initial improvements in skin texture, followed eventually by reduced inflammatory redness and increased dermal firmness.
Looking at reddit topical rapamycin communities, the user experience closely mirrors the clinical timelines. Because rapamycin alters biology at the foundational cellular level, it is not an overnight cosmetic fix. Users on forums like r/Rapamycin and r/SkincareAddiction frequently report sourcing compounded creams from telehealth providers (like Healthspan or RapaShop) or creating DIY topical solutions.
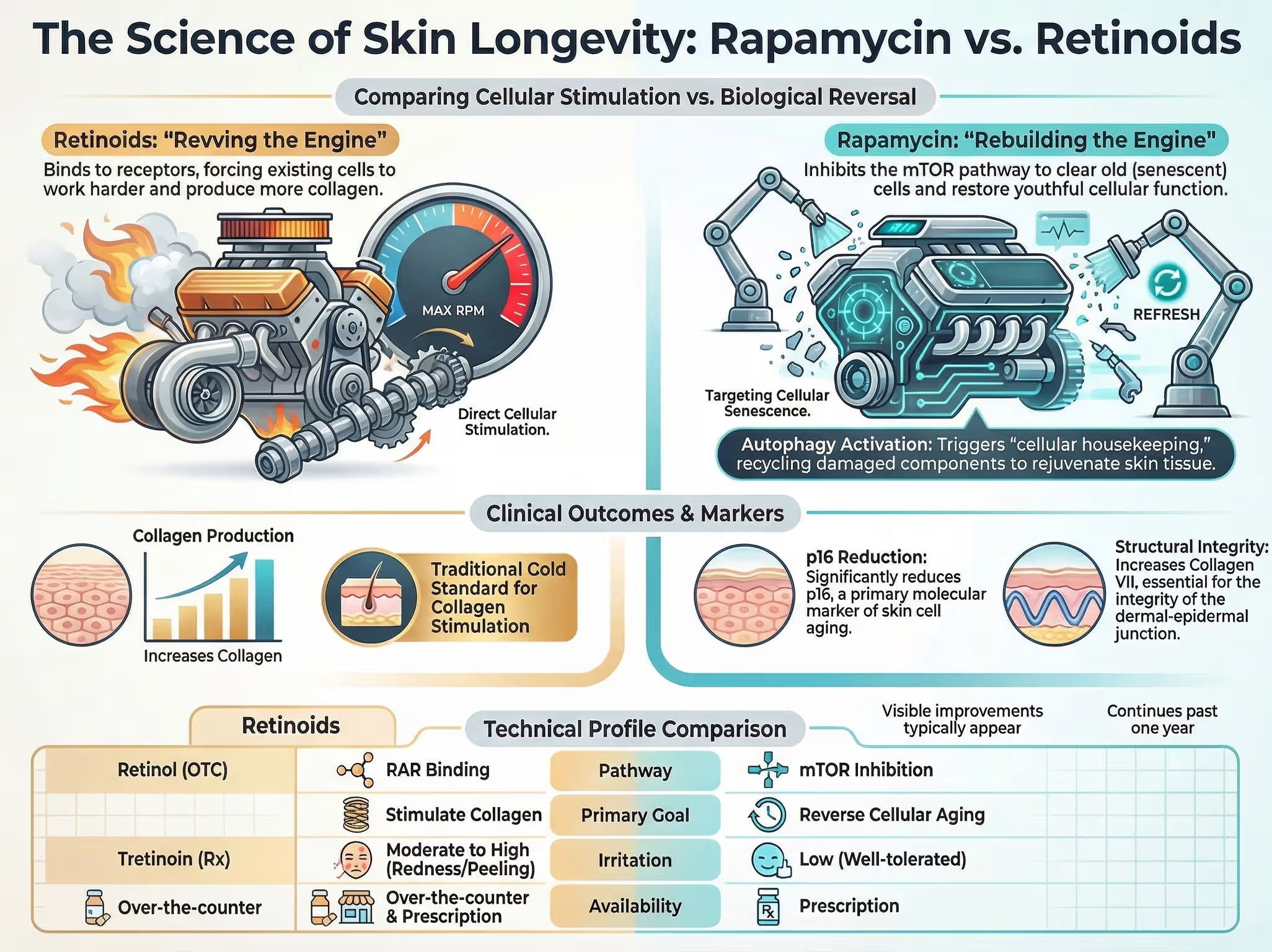
One of the most popular off-label protocols involves combining 1% sirolimus with retinoic acid (tretinoin). Users alternate these treatments to mitigate the redness and sensitivity associated with retinoids. This is a biologically synergistic stack: rapamycin for wrinkles clears the senescent cellular burden and restores the fibroblast’s engine, while the retinoid commands those refreshed cells to produce new collagen.

Does Rapamycin affect hair growth when applied to the scalp?
Yes, emerging anecdotal evidence suggests that topical rapamycin hair protocols can improve scalp health, enhance hair quality, and even reduce graying. By lowering scalp inflammation and preventing follicle stem cell exhaustion, rapamycin creates a highly optimized environment for the hair growth cycle.
While the FDA has not approved rapamycin for hair loss, the biohacking community is actively experimenting with it. Oral rapamycin hair growth benefits have been noted by longevity enthusiasts, but targeted scalp applications offer a direct route. Users report mixing rapamycin solutions with water and applying it to the scalp two to three times weekly. Within months, these users frequently note “better quality hair, more comfortable scalp, [and] new hair less gray”. This aligns biologically with the drug’s capacity to reduce perifollicular inflammation and clear out the senescent cells that otherwise sabotage melanocyte (pigment-producing) function.
What Dosages and Application Protocols Work Best for Skin?
Start with 0.1-1% rapamycin cream (approx. 10 μM) applied evenings, 2-3 times weekly, building to daily on clean skin; pair with SPF due to photosensitivity.
Protocols mimic oral low-dose longevity use: pea-sized amount on face/neck/hands. Trial used 10 μM in emollient base, twice daily. Compounding pharmacies customize strengths; 0.2-1% suits most.
User protocols from forums refine this:
- Week 1-2: 2x/week to test tolerance.
- Ongoing: Daily PM, post-cleanser, pre-moisturizer.
- Cycle: 8 weeks on, 2 off if irritation arises.
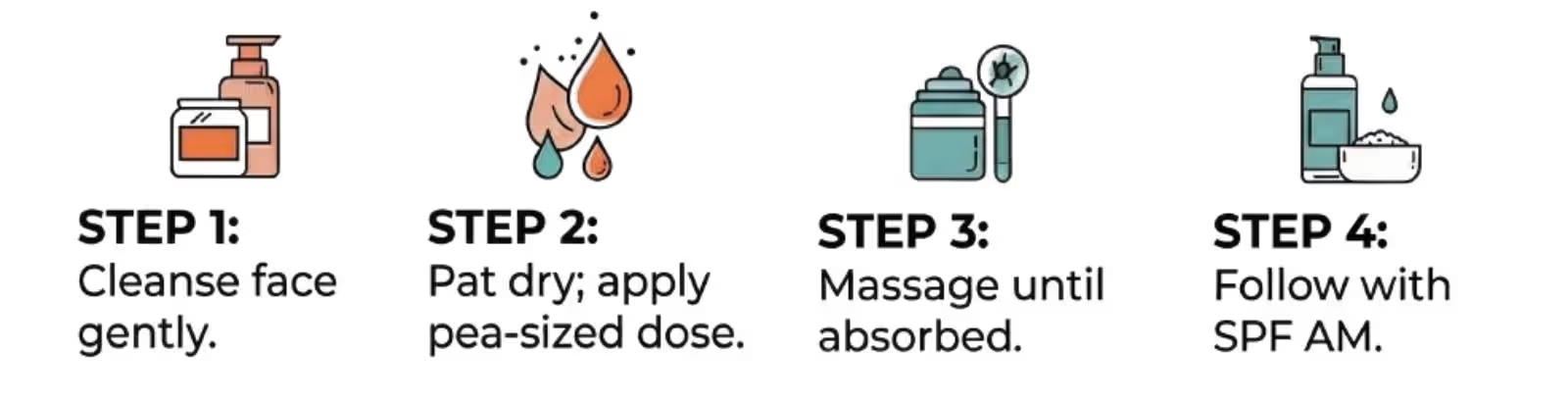
Avoid eyes/mucous membranes. Store refrigerated for stability. Blood tests showed negligible systemic levels, prioritizing local benefits.
Mechanisms of Skin Longevity Therapeutics
| Intervention | Primary Cellular Mechanism | Specific Skin Benefit | Clinical Efficacy Rating |
|---|---|---|---|
| Topical Rapamycin | Inhibits mTORC1, activates autophagy | Decreases p16INK4A, clears senescent fibroblasts, builds Collagen VII | High (Proven in human RCTs) |
| Topical Tretinoin | Binds to Retinoic Acid Receptors (RAR) | Increases cell turnover, forces collagen I and III production | High (Gold Standard) |
| Oral Metformin | Activates AMPK, lowers systemic glucose | Reduces Advanced Glycation End-products (AGEs) to prevent skin stiffening | Moderate (Metabolic optimization) |
Are there side effects or risks with prescription rapamycin?
Oral rapamycin carries systemic risks including immunosuppression, elevated lipids, and mouth ulcers, but topical sirolimus exhibits virtually no systemic absorption. Localized side effects of the cream are generally limited to mild dryness, transient redness, or minor irritation.
When doctors prescribe systemic (oral) mTOR inhibitors for conditions like Tuberous Sclerosis Complex, patients often experience dermatologic adverse events. Up to 70% of these patients develop painful oral ulcers, and 60% experience acneiform (acne-like) eruptions. Oral dosing can also impair wound healing and increase susceptibility to skin infections like folliculitis.
However, sirolimus rapamycin cream applied topically completely changes the safety profile. In the Drexel University trial, researchers confirmed that even after eight months of regular application, systemic absorption of rapamycin into the bloodstream was undetectable. Therefore, the severe immunosuppressive risks associated with oral transplant dosages simply do not apply to the topical anti-aging protocol.

Rapamycin vs. Metformin for longevity: which is better?
Rapamycin is currently viewed as a more promising and potent longevity therapeutic than Metformin. Rapamycin directly inhibits mTOR to drive cellular clearance, whereas Metformin activates AMPK for metabolic optimization, but has shown inconsistent lifespan extension data in healthy models.
Dr. Peter Attia, a prominent longevity physician, recently categorized highly touted anti-aging interventions based on their scientific merit. He categorizes Rapamycin as “promising” due to robust data from the Interventions Testing Program showing consistent lifespan extension across species.
Conversely, Attia downgraded Metformin from “promising” to “fuzzy.” While Metformin excels at lowering advanced glycation end-products (AGEs) and improving insulin resistance in diabetics, recent data questions its ability to extend healthspan in non-diabetic individuals. (For context, Attia categorized Resveratrol as absolute “nonsense,” citing zero reproducible lifespan benefits in wild-type animal models).
For skin longevity, these two drugs offer distinct pathways:
- Rapamycin: A targeted senolytic that clears aged cells and rebuilds the basement membrane (Collagen VII).
- Metformin: A systemic metabolic optimizer that protects existing collagen from being cross-linked and hardened by sugar (glycation).
Conclusion
The narrative around skin aging has permanently shifted from camouflage to cellular repair. By directly inhibiting the mTOR pathway, sirolimus rapamycin cream achieves what traditional cosmetics cannot: the biological clearance of senescent fibroblasts and the restoration of structural collagen proteins like Collagen VII. Whether you are aiming to reverse deep UVA photoaging, reduce inflammatory acne, or explore off-label hair regrowth protocols, rapamycin represents the leading edge of dermatological longevity. Remember to pair it with UV protection and a retinoid protocol to maximize your skin’s biological regeneration.

Yes, clinical trials testing low-dose topical rapamycin for up to eight months demonstrated excellent safety profiles with undetectable systemic absorption. This eliminates the severe immunosuppressive risks associated with oral rapamycin, making localized facial application safe under a doctor’s supervision.
Because rapamycin works by fundamentally reversing cellular senescence and rebuilding the dermal matrix, it operates on a biological timeline. Users and clinical trials report that visible reductions in fine wrinkles, sagging, and skin tone irregularities take between 4 to 8 months to fully materialize.
At the topical concentrations used for anti-aging (0.1% to 0.25%), systemic absorption is so low that immunosuppression is not a clinical concern, unlike with oral transplant dosages.
It softens fine lines and boosts firmness, but pairs best with microneedling for deeper effects.
Yes, many longevity enthusiasts successfully combine the two. Rapamycin works to clear out old, damaged cells and reverse cellular aging, while tretinoin forces the remaining cells to ramp up collagen production. It is heavily advised to alternate application nights to minimize potential skin barrier irritation.
Oral rapamycin targets systemic aging processes throughout the entire body, while topical rapamycin targets skin-specific aging directly at the site of application. Many longevity enthusiasts safely utilize both to maximize their healthspan.
While highly experimental and off-label, users report that topical rapamycin applied to the scalp improves overall hair quality and reduces the rate of graying. The biological rationale is that mTOR inhibition reduces perifollicular inflammation and protects the stem cells responsible for hair growth and pigmentation.
Minimal absorption per blood tests; safer than oral for skin focus.
Reputable compounders like Rapashop.net ensure stability and dosing accuracy.




